SOCIAL MEDIA
Portuguese Medical Association's Scientific Journal
Improving the Care of Hip Fracture Patients Through Orthogeriatrics...
Dear Editor,
We appreciated the recent letter to the editor by Barcelos et al addressing the costs of hip fractures (HF) in postmen...
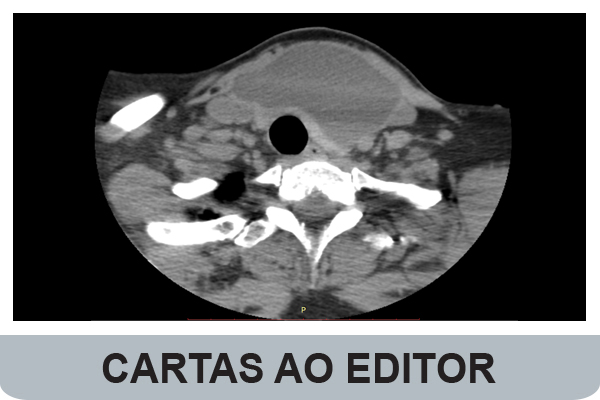
Anterior Cervical Cystic Lymphangioma in an Adult Patient...
Cystic lymphangioma (CL) is a rare benign tumour, located most frequently in the posterior cervical triangle....
read article
Submission to Healthcare Ethics Committees in Portugal: Our Experience...
Dear Editor,
Ethics Committees in health care are instrumental in upholding ethical standards within the life sciences, ensuring th...

Introduction: The paradigm in mental health care is progressively moving towards a recovery-focused perspective. Thus, th...
read article
Polymyalgia Rheumatica After COVID-19 Vaccination: Data from the EudraVigilance Database...
Dear Editor,
Recently, the novel coronavirus (COVID-19) pandemic led to the rapid development of vaccines. Potential side effects h...

How Acta Médica Portuguesa Adjusted to Pandemic Times
A pandemia de COVID-19 tem colocado os sistemas de saúde sob enorme pressão um pouco por todo o mundo, tendo-se verificado nos últimos meses, em Portugal, uma completa reorganização da prestação de cuidados e a constan...
read article