SOCIAL MEDIA
Portuguese Medical Association's Scientific Journal
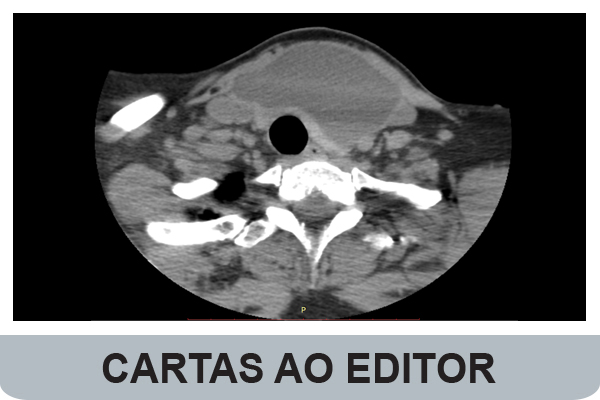
Anterior Cervical Cystic Lymphangioma in an Adult Patient...
Cystic lymphangioma (CL) is a rare benign tumour, located most frequently in the posterior cervical triangle....
read article
Submission to Healthcare Ethics Committees in Portugal: Our Experience...
Dear Editor,
Ethics Committees in health care are instrumental in upholding ethical standards within the life sciences, ensuring th...

Introduction: The paradigm in mental health care is progressively moving towards a recovery-focused perspective. Thus, th...
read article
Polymyalgia Rheumatica After COVID-19 Vaccination: Data from the EudraVigilance Database...
Dear Editor,
Recently, the novel coronavirus (COVID-19) pandemic led to the rapid development of vaccines. Potential side effects h...

Levodopa-Carbidopa: An Unusual Case of Voluntary Drug Intoxication...
Poucos são os casos conhecidos de intoxicação medicamentosa voluntária com levodopa-carbidopa de aç&ati...
read article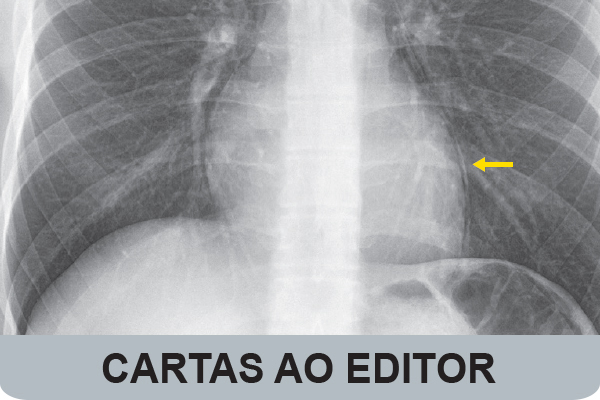
Hamman’s Sign: Rediscovering Cardiac Auscultation Through a Pneumomediastinum...
Pneumomediastinum and pericarditis are distinct etiologies of chest pain with unique mechanisms and specific treatments, but they can exhi...
read article
How Acta Médica Portuguesa Adjusted to Pandemic Times
A pandemia de COVID-19 tem colocado os sistemas de saúde sob enorme pressão um pouco por todo o mundo, tendo-se verificado nos últimos meses, em Portugal, uma completa reorganização da prestação de cuidados e a constan...
read article